
Active surveillance for low-risk papillary thyroid microcarcinomas
Introduction
Papillary thyroid microcarcinoma (PTMC) implies a papillary thyroid carcinoma (PTC) of which maximal diameter is 10 mm or smaller. All PTMCs are not classified as low-risk, because they sometimes have high-risk features such as clinical lymph node metastasis, distant metastasis, and significant extrathyroid extension. PTMCs having high-risk features should be extensively treated as high-risk PTC, including total thyroidectomy, therapeutic/prophylactic lymph node dissection, radioactive iodine (RAI) therapy and thyroid-stimulating hormone (TSH) suppression. At present, how to manage patients with PTMCs with no such high-risk features, i.e., T1aN0M0 PTC, is an important clinical issue because of the recent global increase in patients with such low-risk PTMCs. In this review, we describe about active surveillance of low-risk PTMC. Therefore, the word “PTMC” in this manuscript means not all PTMCs but low-risk PTMCs only. Also, there was insufficient evidence to adopt active surveillance to manage high-risk PTMCs.
Formerly, PTMCs were found at autopsies as latent carcinomas. Among adult subjects who died of non-thyroid diseases, the incidence of latent PTMCs measuring 3–10 mm (which are detectable on ultrasound) is high at 0.5–5.2% (1). Recent improvements in the resolving power of ultrasound and the establishment of an ultrasound-guided fine-needle aspiration cytology (FNAC) technique enabled the easy detection and diagnosis of PTMCs with thyroid screenings and by imaging tests for other diseases, e.g., ultrasound examination for arteriosclerosis and chest computed tomography (CT) scans for diseases of lungs, including lung metastasis of other carcinomas.
Takebe et al. performed thyroid screening using ultrasound for women >30 years old who underwent breast cancer screening and they performed FNAC for the detected thyroid nodules. They detected and cytologically diagnosed thyroid carcinoma in 3.5% of them (2). The prevalence was similar to that reported in autopsy studies and as much as 1,000 times higher than that of thyroid carcinoma in Japanese women of the time (3.1 per 100,000 population). An important question thus arose; i.e., whether the detection of such PTMCs and surgery for them is truly beneficial for patients.
In 1993, Akira Miyauchi at Kuma Hospital (Kobe, Japan) proposed and initiated a program of active surveillance for PTMCs after a prospective clinical trial was approved by the hospital’s medical staff committee (equivalent to an ethics committee). Thereafter, Miyauchi et al. introduced various insights into the active surveillance of PTMCs (3). Before the study’s proposal, Dr. Miyauchi developed the following hypotheses: (I) most PTMCs do not grow or they grow very slowly, (II) for evaluating whether individual PTMC cases have growth activity, active surveillance is only the strategy, (III) it is not late to perform a conversion surgery when progression signs such as tumor growth or novel lymph node metastasis appeared, and (IV) it is more harm than good to routinely perform immediate surgery for PTMCs (4). In 1995, Japan’s Cancer Institute Hospital also started active surveillance subject to the same policy. These two institutions have published many reports on active surveillance since then.
Since favorable outcomes of PTMC patients who underwent active surveillance have been published, this management was accepted as an approach for PTMC in the guidelines conducted by the Japan Association of Endocrine Surgeons and the Japanese Society of Thyroid Surgery (these two entities were unified to form the Japan Association of Endocrine Surgery, or JAES) (5). The 2018 revision of the JAES guidelines recommend this observational management more positively (6). In addition, the 2015 American Thyroid Association (ATA) guidelines state that the active surveillance of PTMCs is one of the management strategies (7).
The increasing incidence and unchanged rate of mortality of thyroid carcinoma
With the development of ultrasound and the ultrasound-guided FNAC technique, thyroid carcinomas—especially PTMCs—are now easily detected, diagnosed, and treated. However, a negative effect of this new ease of detection has been reported in various countries; harmless PTCs have been detected, diagnosed, and treated by surgery that was unnecessary. In the U.S., the incidence of thyroid carcinoma increased by 2.4-fold between 1973 and 2002 and by 2.9-fold between 1975 and 2009, but the mortality rate was stable throughout this period (8,9). South Korea performed a national screening program for thyroid cancer by ultrasound and cytology, resulting in even more dramatic difference: the thyroid carcinoma’s incidence rapidly increased by 15 times between 1993 and 2011, but its rate of mortality did not decrease, and the number of patients who suffered from surgical complications increased significantly (10). Similar phenomena were detected in several other countries such as Italy, the UK, Australia, and the Nordic countries (11). These data indicate that numerous harmless PTCs were detected and diagnosed, resulting in unnecessary surgery for patients worldwide.
Adverse events of surgery for PTMC
Surgery for a PTMC is not technically difficult. However, the incidence of adverse events of any surgery is not zero. A South Korean study stated that many patients who underwent surgery for thyroid carcinoma suffered vocal cord paralysis and hypoparathyroidism (10). Oda et al. compared the incidences of various unfavorable events between PTMC patients who chose active surveillance (including those who underwent conversion surgery later) (the active surveillance group), and those who chose immediate surgery (the surgery group) (12). The incidences of transient hypoparathyroidism in the surgery group and active surveillance group were 16.7% and 2.8%, respectively (P<0.0001). Also, the incidences of permanent hypoparathyroidism in these groups were 1.6% and 0.08% (P<0.0001), respectively. The incidence of transient vocal cord paralysis in the surgery group was 4.1%, and that in the active surveillance group was much lower at 0.6% (P<0.0001). In addition, permanent vocal cord paralysis due to recurrent laryngeal nerve injury occurred in 2 patients (0.2%) in the surgery group. The surgeries were all conducted at Kuma Hospital, which is a specialized hospital for the thyroid; the surgeons were highly experienced endocrine surgeons. Had non-experts performed the surgeries, the incidences of these adverse events would have been much higher. This issue is very important when considering the benefits of active surveillance for PTMC.
Indications for surgery in PTMCs
The initial patient selection is very important for active surveillance. Table 1 lists the indications for PTMC surgery. PTMCs that are positive for clinical node metastasis or distant metastasis (although this is extremely rare), symptomatic PTMCs, and PTMCs with aggressive features on cytology are strong candidates for immediate surgery.
Table 1
| Type | Indications of surgery |
|---|---|
| Clinically high-risk features | Positive for clinical lymph node or distant metastasis (very rare) |
| Signs or symptoms of invasion of the recurrent laryngeal nerve or trachea | |
| High-grade malignancy on cytology (very rare) | |
| A feature unsuitable for active surveillance | Tumors possibly invading the trachea or recurrent laryngeal nerve |
| Features preferable for surgery | Association of other significant indication(s) for thyroid or parathyroid diseases |
| No evidence for active surveillance | Patients <20 years old |
PTMC, papillary thyroid microcarcinoma.
PTMCs that may be invading (or may in the near future invade) the trachea and/or the recurrent laryngeal nerve because of their close location to these vital organs are not suitable for active surveillance, although the progression of the disease cannot be reliably predicted (Table 1). These features do not directly indicate aggressive behaviors, but if a tumor grows and invades the trachea and/or the recurrent laryngeal nerve, the patient’s quality of life (QoL) could be significantly damaged even though surgical treatment is performed at that moment.
For evaluating tracheal invasion, the angles between tumor surface and the tracheal cartilage and tumor surface is helpful (13): in that study, 24% of PTMCs ≥7 mm forming obtuse angles had significant tracheal invasion that required laminate or window resection for curative surgery, but none of the patients whose PTMCs did not meet those criteria but were attached to the trachea were candidates for immediate surgery.
For the evaluation of recurrent laryngeal nerve invasion, it is important whether or not a normal rim is present between the thyroid capsule and the tumor surface (10): in that study, 9% of PTMCs ≥7 mm without a normal rim showed invasion to the nerve and, for curative surgery, partial layer resection or resection of the nerve with anastomosis to the ansa cervicalis was required (13). If a normal rim is present, immediate surgery is not necessary and the patient can undergo active surveillance. PTMCs suspected of invasion to the anterior or lateral capsule of the thyroid can undergo active surveillance, because conversion surgery would be easy without damaging the patient’s QoL.
If PTMCs are associated with significant thyroid or parathyroid disease indicated for surgery, such as significant thyroid nodules, symptomatic hyperparathyroidism, or Graves disease, a combined surgical treatment of these diseases is considered. To date, no evidence is available regarding the outcomes of active surveillance for PTMC in pediatric patients.
Patients with family history of differentiated thyroid carcinoma or tumor multiplicity can be candidates for active surveillance. Indeed, they may moderately affect patients’ prognoses. However, the total thyroidectomy should generally be done for these patients would increase the rate of adverse events from surgery, e.g., recurrent laryngeal nerve paralysis and permanent hypoparathyroidism. In our experience at Kuma Hospital, a positive family history of PTC and multiple PTMCs were not significant factors for disease progression on active surveillance, as described below.
The active surveillance program at Kuma Hospital
Our active surveillance program starts from the cytological diagnosis of PTC for suspicious nodules ≥5 mm [subject to the recommendation by the Japan Association of Breast and Thyroid Sonology (14)]. This significantly differs from the ATA’s 2015 guidelines, which do not recommend FNAC for nodules ≤10 mm unless they have malignant features such as patient symptoms and lymph node/distant metastasis (7). This may be because of an assumption that patients in the U.S. will be reluctant to accept active surveillance. We routinely perform FNAC and tell the patients their diagnoses. If we do not perform FNAC for suspicious small lesions, the patients may possibly visit other hospitals, cytologically diagnosed as PTMC, and undergo unneeded surgery. Our hospital could also be subjected to bad publicity that we ‘overlooked thyroid carcinomas’. These events would be unfavorable for patients and our hospital. We think that periodical check-up studies are also necessary for suspicious small lesions, since some of them might progress. Without the use of FNAC-based diagnoses, this would be almost impossible.
We therefore present two management options to the patients—active surveillance and immediate surgery. Of course, it is essentially each patient’s choice whether he or she will undergo active surveillance or immediate surgery. In the past, we presented these two management options equally to the patients. However, since a significant amount of favorable data about active surveillance has accumulated, we now recommend active surveillance as the first-line management to the patients, though we still explain the immediate surgery option as well. The proportion of patients who choose active surveillance has gradually increased over time, and now the majority of the patients at our hospital (>95%) choose active surveillance. Patients who choose active surveillance can also freely change their preference and can undergo conversion surgery at any time during active surveillance, but the incidence of such patients has significantly decreased over time (manuscript submitted).
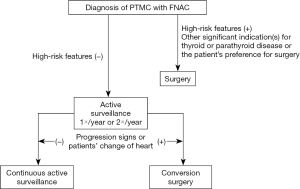
Figure 1 is a simple algorithm for active surveillance. Patients who choose active surveillance are asked to visit our clinic 6 months later and ≥1×/year thereafter for a check-up with an ultrasound examination and thyroid function blood tests. An increase in the tumor size by ≥3 mm compared with the size at the initiation of active surveillance is judged as enlargement. However, if the patient prefers, we perform continuous active surveillance and recommend surgery if the tumor size reaches 13 mm. This is because 13 mm is the maximum size suitable for active surveillance in our inclusion criteria. If a lymph node suspected of metastasis has newly appeared, we perform FNAC and measure the thyroglobulin level of 1 mL saline where the needles used for FNAC were washed. If metastasis is diagnosed, we perform conversion surgery, which is essentially a total thyroidectomy with neck dissection of the central compartment and the ipsilateral lateral neck compartment (4).
Patients’ outcomes of active surveillance in Japan
In the first [2003] report about active surveillance at Kuma Hospital, we noted that more than 70% of the PTMCs were stable or even shrunk. Regarding node metastasis, novel appearance of metastatic nodes was seen only in 1.2% of patients (15). According to the second [2010] report, tumor enlargement rates (by ≥3 mm) were 6.4% and 15.9% at 5- and 10-year observation, respectively. Lymph node metastasis newly appeared in 1.5% and 3.4% of patients at 5- and 10-year observation, respectively (16). In 2014, we showed that, by enrolling 1,235 patients, the 5- and 10-year cumulative enlargement rates were 4.9% and 8.0%, and cumulative rates of lymph node metastasis appearance were 1.7% and 3.8%, respectively (17). Also, patients’ ages at diagnosis were inversely related to tumor enlargement rates: the 10-year rates were 12.1%, 9.1%, and 4.1% for patients aged <40, 40–59, and ≥60 years, respectively. Similarly, 10-year rates of novel appearance of node metastasis were 16.1%, 2.3%, and 0.5% for patients aged <40, 40–59, and ≥60 years, respectively. A multivariate analysis revealed that young age (<40 years) was the only independent predictor of PTMC progression, but family history of differentiated thyroid carcinoma and multiplicity were not (17). These findings indicate that PTMC patients with tumor multiplicity or a family history can also be candidates for active surveillance.
In 2010, Sugitani et al. (18) at the Cancer Institute Hospital showed that 7% of PTMCs showed tumor enlargement and novel appearance of node metastasis was seen only in 1% of them. They published a second report in 2019 showing similar data for 360 patients (19). In the latter study, they also included preliminary outcomes of active surveillance for small numbers of T1bN0M0 PTCs ≤16 mm.
Outcomes of PTMCs under active surveillance in other countries
The Memorial Sloan Kettering Cancer Center (New York, NY, USA) published a clinical framework of active surveillance in collaboration with Kuma Hospital in 2016 (20). They classified PTMCs into three categories, which are actually similar to the indications and contraindications for active surveillance of PTMCs used at Kuma Hospital: ideal, appropriate, and inappropriate for active surveillance. The inappropriate characteristics of active surveillance are as follows: (I) evidence of aggressive cytology, (II) subcapsular locations adjacent to the recurrent laryngeal nerve, (III) evidence of extrathyroidal extension, (IV) clinical evidence of invasion of the recurrent laryngeal nerve or trachea, (V) N1 disease, (VI) M1 disease, and (VII) a documented ≥3-mm increase in the size of a confirmed PTC tumor.
Thereafter, Tuttle et al. (21) enrolled 291 patients with PTCs measuring ≤15 mm in a prospective study. They evaluated tumor enlargement not only by maximal diameter but also by tumor volume. They demonstrated that 12.7% of the tumors increased in volume by >50%, while only 3.8% of the tumors increased in maximal diameter by ≥3 mm. Based on these results, they concluded that the evaluation of tumor volume more keenly reflects tumor growth and is more useful to select PTMCs with high growth activity than the evaluation of maximal diameter.
Studies from South Korea that included ‘passive surveillance’ were published in 2017–2018 (22,23). A multicenter retrospective study enrolling 370 patients (median follow-up period, 32.5 months) was published in 2018 (23): the incidence of enlargement was 23.2% based on a volume increase ≥50%, and the incidence was 3.5% based on a size increase ≥3 mm, which was similar to the data in the Tuttle et al. investigation. However, this South Korean study described a rather high incidence of conversion surgery, at 15.7%.
Favorable outcomes of patients who undergo active surveillance have also been reported from Latin America (24,25) and Italy (26), although the numbers of enrolled patients were smaller in these studies.
Table 2 summarizes the results of representative studies. In all of the studies, none of the patients showed fatal metastasis or died of thyroid carcinoma during the follow-up or after conversion surgery, which is also clearly described in a meta-analysis (27).
Table 2
| Affiliation | Study design | No. of patients | Mean follow-up period | Rate of size enlargement ≥3 mm (%) | Rate of appearance of node metastasis (%) | No. of patients who underwent conversion surgery | No. of patients who died of thyroid carcinoma |
|---|---|---|---|---|---|---|---|
| Kuma Hospital (16) | Prospective | 340 | 74 [18–187] months | 6.4% at 5-yr follow-up | 1.4% at 5-yr follow-up | 109 (32%) | 0 |
| Kuma Hospital (17) | Prospective | 1,235 | 60 [18–228] months | 8.0% at 10-yr follow-up | 3.8% at 10-yr follow-up | 191 (16%) | 0 |
| Cancer Institute Hospital (18) | Prospective | 230 | 5 [1–17] yrs | 7% after follow-up | 1.3% after follow-up | 16 (7%) | 0 |
| Cancer Institute Hospital* (19) | Prospective | 360 | 7.9 [1–17] yrs | 8% after follow-up | 1% after follow-up | NA | 0 |
| Multicenter study (South Korea) (23) | Retrospective | 370 | 33 months | 6.4% at 5-yr follow-up | 1.4% after follow-up | 58 (16%) | 0 |
| Memorial Sloan Kettering Cancer Center**(21) | Prospective | 290 | 25 [6–166] months | 12.1% at 5-yr follow-up | NA | 10 (3%) | 0 |
| Universidad de Antioquia (24) | Prospective | 57 | 13 [0–57] months | 10% at 1-yr follow-up | NA | 5 (9%) | 0 |
| University of Buenos Aires** (25) | Prospective | 34 | 42 [7–120] months | 17% after follow-up | NA | 10 (29%) | 0 |
| University Hospital of Pisa*** (26) | Prospective | 93 | 19 [6–54] months | 3% after follow-up | NA | 3 (3%) | 0 |
*, Data about T1aN0M0 patients were extracted. **, Enrolled patients with PTC ≤15 mm. ***, Enrolled patients with PTC ≤13 mm. PTMC, papillary thyroid microcarcinoma; NA, not available.
Which is better for evaluating tumor growth: the maximal diameter or the tumor volume?
The following question thus arises: which is better for evaluating tumor growth, the maximal diameter or the tumor volume? Research groups in the U.S. and South Korea recommended the evaluation based on tumor volume because this can more rapidly identify PTMCs with high growth activity (21-23). Japanese physicians have traditionally used the maximal tumor diameter increase by ≥3 mm for tumor enlargement.
If a tumor measuring 6 mm3 grows to 7 mm3, the volume increase would be 59%, indicating that this tumor would be judged as enlarged in the Tuttle et al. and Oh et al. studies (21,23). This example’s status is definitely too early to decide whether conversion surgery is necessary. In Japanese institutions such as Kuma Hospital and the Cancer Institute Hospital, size enlargement by ≥3 mm has been adopted from the initiation of active surveillance. With the use of this criterion, none of the patients showed distant metastasis or died of thyroid carcinoma during active surveillance. In addition, none of the patients who underwent conversion surgery for various reasons, including tumor enlargement, showed significant recurrence or died of thyroid carcinoma, suggesting that the definition used in Japanese institutions is more appropriate. Moreover, as described below, the growth activity of PTMCs is not uniform, indicating that a too-sensitive criterion for conversion surgery results in unnecessary treatment for PTMC patients. However, the time limit for conversion surgery remains to be clarified.
For evaluations of the changes in tumor volume, the tumor volume doubling-time (or doubling rate) is useful, as described in the next part
The natural history of PTMCs
Miyauchi et al. (28) investigated the rate of PTMC progression when patients underwent active surveillance for 10 years for age-decade groups. They used these rates and calculated the lifetime probability of PTMC enlargement for each age-decade group, as follows: 48.6% of patients in their 20s, 25.3% of patients in their 30s, 20.9% of patients in their 40s, 10.3% of patients in their 50s, 8.2% of patients in their 60s, and 3.5% of patients in their 70s. Patients aged at 20s and 30s might be considered too high lifetime probabilities of PTMC progression, but in other words, more than one-half of patients in their 20s and three-quarters of patients in their 30s could avoid conversion surgery in their lifetime. We thus conclude that young patients (i.e., in their 20s or 30s) can also be candidates for active surveillance.
Miyauchi et al. (29,30) proposed the doubling rate to evaluate the changes in tumor volume, the inverse of the doubling time. The doubling time is an excellent tool for evaluations of change in tumor volume, but it includes two problem points: (I) the doubling times of tumors shrinking over time are given in negative values (<0). When evaluating the growth activity of tumors, discontinuity occurs when tumors with a negative doubling time are included. (II) The magnitude of the doubling time is opposite that of the tumor growth rate. If we employ the doubling rate, these problems can easily be solved. The doubling rate indicates the number of doublings (or halvings, if it is a negative value) of the tumor volume per unit of time.
Miyauchi et al. then calculated the tumor volume doubling rates (/year) of PTMCs that underwent active surveillance. These rates were and classified into four categories: >0.5 (rather rapid growth), 0.1 to 0.5 (slow growth), –0.1 to 0.1 (stable), and less than –0.1 (decrease in growth). They evaluated the doubling rates for 169 PTMCs and of these, 5, 38, 97, and 29 showed rather rapid growth, slow growth, stable status, and a decrease in growth, respectively (30). During active surveillance, 17% of the PTMCs had a doubling rate less than –0.1 because their tumor volumes decreased over time. The incidence of PTMCs with rather rapid or slow growth significantly decreased with advancing age as follows: 40%, 29%, and 17% in patients aged <40, 40–59, and ≥60 years, respectively (30).
Miyauchi et al. (30) also estimated the ‘hypothetical’ tumor volume doubling rate of PTMCs before presentation. Suppose that one cancer cell having 10 µm as a maximal diameter had already been present at the time of patient’s birth that constantly grew. Therefore, this value showed the lowest growth rate. In real world, since a cancer cell should appear later, the actual doubling rate of PTMC before presentation would be higher than the hypothetical doubling rate. Despite that, the estimated hypothetical doubling rates before presentation were much higher than doubling rates during active surveillance after presentation (30). This strongly suggests that PTMCs more rapidly grow before presentation. Then, the growth activity significantly diminished after presentation, which can be considered as a typical natural course of PTMCs.
More recently, Ito et al. investigated the change in growth activity evaluated based on the tumor volume doubling rate before and after the tumor reached the enlargement points, i.e., a size increase by ≥3 mm and a tumor volume increase by ≥50% (31). The doubling rates after the enlargement point based on size increase by ≥3 mm and tumor volume enlargement ≥50% were significantly lower than those before the enlargement point (–0.091/year vs. 0.509/year, P<0.0001 for size enlargement and –0.058/year vs. 0.380/year, P<0.0001 for tumor volume enlargement). Based on the tumor size and the tumor volume, only 7.7% and 3.8% of the tumors continued to rather rapidly enlarge (doubling rate >0.5/year), respectively. That study also reported that 47.4% and 36.1% of the tumors even shrank (doubling rates <–0.1/year) after the enlargement points based on tumor size and tumor volume, respectively. These findings are consistent with Miyauchi’s above-mentioned hypothesis and suggest that performing conversion surgery immediately after tumor enlargement may be too hasty, and for patients who do not prefer surgery, continuing active surveillance may be better in order to avoid unnecessary surgery.
Other clinical questions
The relationship between PTMC and pregnancy
A high amount of human chorionic gonadotropin (which has TSH-like activity) is secreted during pregnancy, which might stimulate the growth of a PTMC. For PTMCs in women of reproductive age, it is thus important to consider whether active surveillance is indicated. Ito et al. (32) investigated the records of the change in size of PTMCs in young women, and they observed that only 8% (4 of the 51 patients) of PTMCs enlarged by ≥3 mm during pregnancy. Of these, two underwent conversion surgery after delivery and they did not show significant recurrence/metastasis after surgery. The remaining two were continued active surveillance because their PTMCs came to be stable after delivery. Therefore, PTMCs in young women can also be candidates for active surveillance.
Relationship between PMTC growth and ultrasound findings
Fukuoka et al. demonstrated that PTMCs with rich vascularity or with microcalcification only were more likely to grow than those showing poor vascularity and/or a high degree of calcification (33). However, 61.4% of PTMCs that had a rich vascularity at the beginning had decreased vascularity during active surveillance. Also, 51.8% of the tumors had increased calcification at the 10-year follow-up. A high degree of calcification and poor vascularity at the last examination were each inversely related to PTMC progression, but no patients in their series demonstrated a life-threatening metastasis or died of thyroid carcinoma not only during active surveillance but also after conversion surgery. It is therefore concluded that rich vascularity and microcalcification are not be conditions for immediate surgery.
Differences in medical costs between active surveillance and immediate surgery
Oda et al. investigated the difference in costs subject to the Japanese health care insurance system between immediate surgery and active surveillance. The 10-year cost of immediate surgery was 4.1 times higher than that of active surveillance (928,094 vs. 225,695 yen/patient) (34). This analysis, based on the actual management flow at Kuma Hospital, included the cost of conversion surgery after the active surveillance and the costs of surgery for recurred lesions and various postoperative managements for patients who underwent immediate surgery. Also, a report from Hong Kong showed the cost-effectiveness of active surveillance as compared with immediate surgery (35). In the U.S., there is a report demonstrating that immediate hemithyroidectomy was superior to active surveillance for cost-effectiveness, but their methods of analyses included many assumptions and were very difficult to understand (36). The costs of active surveillance and immediate surgery vary among countries, and the cost-effectiveness should be considered for each country.
The effects of TSH suppression on PTMC progression
Controversial findings were reported regarding the relationship between TSH suppression and PTMC progression. Sugitani et al. (37) showed that TSH levels are not correlated with PTMC progression, whereas Kim et al. (38) showed a relationship between sustained serum TSH elevation and PTMC progression. Ito et al. (16) noted that in younger patients who underwent TSH suppression, PTMCs only occasionally grew, although the PTMCs in younger patients normally have higher growth activity than those in older patients. However, the number of patients who underwent TSH suppression was small in that study, and further studies enrolling larger numbers of patients should be done for drawing any definitive conclusions. However, a low-normal setting for the serum TSH level might be a favorable for active surveillance especially in younger patients, since these patients tend to show a higher rate of disease progression.
Anxiety in patients and physicians
QoL is a very important issue for patients suffering carcinoma. Since thyroid carcinoma usually has a course of long duration, physicians should take care how to maintain or improve QoL of thyroid carcinoma patients. To date, no studies have been published about comprehensive QoL of patients with PTMC who undergo active surveillance, but patients’ anxiety for active surveillance has been studied by some institutions.
According to two Australian studies, many physicians hesitate active surveillance because of their anxiety (39,40), but such anxiety would arise mainly from a lack of experience. At Kuma Hospital, the incidence of patients who chose active surveillance was only 30% between 1993 and 1997. However, the incidence significantly elevated over time and reached 88% in 2014 and ≥95% in 2018 (41). This increase occurred because the safety and effectiveness of active surveillance were firmly established over this period, and because physicians realized that unfavorable events such as permanent vocal cord paralysis and hypoparathyroidism cannot be avoided completely even by skillful surgeons (17). In addition, it is quite likely that physicians’ anxiety can influence their patients’ level of anxiety.
Conflicting data about patients’ anxiety have been obtained in several studies, although some of the studies enrolled small numbers of cases with comparably short follow-ups (42-44). According to a joint study between the Dartmouth Institute in the U.S. and Kuma Hospital, 37% of patients who were on active surveillance in Kuma Hospital had worried sometimes (or even more often) about their cancer. However, 60% of the patients described a decrease in their worrying over time. Also, as much as 80% of the patients agreed or strongly agreed that their decision to undergo active surveillance matched their personal values. Very importantly, as much as 83% of patients agreed or strongly agreed that active surveillance was the best decision for themselves (45). These favorable results might be due to the confident attitude of the attending physicians.
In Kuma Hospital, a brochure that explains not only favorable outcomes but also safety of active surveillance is handed to the patients having nodules suspected of PTMC before FNAC rather than at the time when they are told their cytological diagnosis. For patients who are undergoing continuous active surveillance, another brochure is prepared to eliminate or alleviate their anxiety. Also, the Memorial Sloan Kettering Cancer Center and a Korean team developed an aid named “Thyroid Cancer Treatment Choice” to support conversations between patients and physicians (46). They reported that this aid is significantly useful to explain various issues for active surveillance to patients.
Biological markers for predicting the growth of PTMCs
Using surgical specimens, Hirokawa et al. (47) observed that the Ki-67 labeling index in enlarged PTMCs was significantly higher than that in PTMCs that did not enlarge but were treated surgically. The expression of Ki-67 is heterogeneous, and the labeling index was calculated in hot spots; thus, this strategy cannot be used on cytological specimens or be used to discriminate PTMCs that can be expected to grow. At present, no molecular or pathological markers are used to predict PTMC progression using cytological specimens. TERT mutations associated with BRAF mutations predict a poor prognosis of PTC; however, none of the PTMCs, including those showing enlargement, had TERT mutations (48). To date, therefore, continuous active surveillance is the only method to identify PTMCs with constant growth.
Educating patients and physicians to implement active surveillance
Active surveillance for properly selected patients with low-risk PTMCs is thus superior to immediate surgery in light of the oncological outcomes, safety, incidences of unfavorable events, and medical costs. However, this management option started in 1993, only 27 years ago, and was recognized in the Japanese and American guidelines only about 5 years ago. Therefore, the vast majority of the patients with the disease as well as most physicians might think that surgical resection is the only treatment, or they may not have heard of this new observational management option. In order to implement this management in clinical practice, it is very important to educate patients, the physicians taking care of them, and the general public. Sonographers with experience with the thyroid and neck are needed for the diagnoses and follow-up examinations. It is also necessary to provide aid to patients to avoid dropouts from active surveillance, because a small portion of PTMCs do progress over time. In order to avoid dropouts, the education of patients has been found to be very important (49).
We routinely perform cytological examinations for suspicious nodules and tell the patients at the diagnosis, and this is likely to help prevent dropouts. At Kuma Hospital in April 2013, we created a reminder system about regular check-ups for non-show patients, sending reminder letters to those who have not seen their physicians for >18 months. At our institution, the rate of lost to follow-up is <10% (our unpublished data).
Conclusions
Active surveillance is an excellent strategy for patients with low-risk PTMCs, based on the oncological safety, low incidences of unfavorable events, and lower medical costs. We can therefore conclude that active surveillance is suitable as the first-line management for PTMCs (50-52). In Japan, based on a questionnaire survey to member institutions of the JAES and JSTS, 53.8% of the patients with low-risk PTMCs underwent active surveillance during three consecutive months in 2018 (53), indicating that this strategy is prevailing in Japanese institutions. We hope that active surveillance will be adopted as an excellent and established management strategy worldwide.
Acknowledgments
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editors (Marcin Barczyński and Maurizio Iacobone) for the series “Recent Challenges in the Management of Thyroid Tumors” published in Annals of Thyroid. The article has undergone external peer review.
Conflicts of Interest: Both authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/aot-2020-rcmtt-06). The series “Recent Challenges in the Management of Thyroid Tumors” was commissioned by the editorial office without any funding or sponsorship. AM serves as an unpaid editorial board member of Annals of Thyroid from Jul 2019 to Jun 2020. The author has no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Ito Y, Miyauchi A. Prognostic factors and therapeutic strategies for differentiated carcinomas of the thyroid. Endocr J 2009;56:177-92. [Crossref] [PubMed]
- Takebe K, Date M, Yamamoto N. Mass screening for thyroid cancer with ultrasonography. Karkinos 1994;7:309-17.
- Miyauchi A, Ito Y, Oda H. Insights into the management of papillary microcarcinoma of the thyroid. Thyroid 2018;28:23-31. [Crossref] [PubMed]
- Miyauchi A. Clinical trials of active surveillance of papillary microcarcinoma of the thyroid. World J Surg 2016;40:516-22. [Crossref] [PubMed]
- Takami H, Ito Y, Okamoto T, et al. Therapeutic strategy for differentiated thyroid carcinoma in Japan based on a newly established guideline managed by Japanese Society of Thyroid Surgeons and Japanese Association of Endocrine Surgeons. World J Surg 2011;35:111-21. [Crossref] [PubMed]
- Japanese Society of Thyroid Surgery, Japan Association of Endocrine Surgeons. Guidelines for the Management of Thyroid Tumors. 2nd ed. Tokyo: Official Journal of the Japan Association of Endocrine Surgery, 2018.
- Haugen BR, Alexander EK, Bible KC, et al. 2015 American Thyroid Association management guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: The American Thyroid Association guidelines task force on thyroid nodules and differentiated thyroid cancer. Thyroid 2016;26:1-133. [Crossref] [PubMed]
- Davies L, Welch HG. Increasing incidence of thyroid cancer in the United States, 1973-2002. JAMA 2006;295:2164-7. [Crossref] [PubMed]
- Davies L, Welch HG. Current thyroid cancer trends in the United States. JAMA Otolaryngol Head Neck Surg 2014;140:317-22. [Crossref] [PubMed]
- Ahn HS, Kim HJ, Welch HG. Korea's thyroid-cancer "epidemic"—Screening and overdiagnosis. N Engl J Med 2014;371:1765-7. [Crossref] [PubMed]
- Vaccarella S, Franceschi W, Bray F, et al. Worldwide thyroid-cancer epidemic? The increasing impact of overdiagnosis. N Engl J Med 2016;375:614-7. [Crossref] [PubMed]
- Oda H, Miyauchi A, Ito Y, et al. Incidences of unfavorable events in the management of low-risk papillary microcarcinoma of the thyroid by active surveillance versus immediate surgery. Thyroid 2016;26:150-5. [Crossref] [PubMed]
- Ito Y, Miyauchi A, Oda H, et al. Revisiting low-risk thyroid papillary microcarcinomas resected without observation: was immediate surgery necessary? World J Surg 2016;40:523-8. [Crossref] [PubMed]
- Masafumi K, Shinichi S. Japan Association of Breast and Thyroid Sonology. Thyroid ultrasound—a guidebook for diagnosis and management. 3rd ed. Tokyo: Nankodo, 2016.
- Ito Y, Uruno T, Nakano K, et al. An observation trial without surgical treatment in patients with papillary microcarcinoma of the thyroid. Thyroid 2003;13:381-7. [Crossref] [PubMed]
- Ito Y, Miyauchi A, Inoue H, et al. An observational trial for papillary thyroid microcarcinoma in Japanese patients. World J Surg 2010;34:28-35. [Crossref] [PubMed]
- Ito Y, Miyauchi A, Kihara M, et al. Patient age is significantly related to the progression of papillary microcarcinoma of the thyroid under observation. Thyroid 2014;24:27-34. [Crossref] [PubMed]
- Sugitani I, Toda K, Yamada K, et al. Three distinctly different kinds of papillary thyroid microcarcinoma should be recognized: our treatment strategies and outcomes. World J Surg 2010;34:1222-31. [Crossref] [PubMed]
- Sakai T, Sugitani I, Ebina A, et al. Active surveillance for T1bN0M0 papillary thyroid carcinoma. Thyroid 2019;29:59-63. [Crossref] [PubMed]
- Brito JP, Ito Y, Miyauchi A, et al. A clinical framework to facilitate risk stratification when considering an active surveillance alternative to immediate biopsy and surgery in papillary microcarcinoma. Thyroid 2016;26:144-9. [Crossref] [PubMed]
- Tuttle RM, Fagin JA, Minkowitz G, et al. Natural history and tumor volume kinetics of papillary thyroid cancers during active surveillance. JAMA Otolaryngol Head Neck Surg 2017;143:1015-20. [Crossref] [PubMed]
- Kwon H, Oh HS, Kim M, et al. Active surveillance for patients with papillary thyroid microcarcinoma: a single center's experience in Korea. J Clin Endocrinol Metab 2017;102:1917-25. [Crossref] [PubMed]
- Oh HS, Ha J, Kim HI, et al. Active surveillance of low-risk papillary thyroid microcarcinoma: a multi-center cohort study in Korea. Thyroid 2018;28:1587-94. [Crossref] [PubMed]
- Sanabria A. Active surveillance in thyroid microcarcinoma in a Latin-American cohort. JAMA Otolaryngol Head Neck Surg 2018;144:947-8. [Crossref] [PubMed]
- Smulever A, Pitoia F. Active surveillance in papillary thyroid carcinoma: not easily accepted but possible in Latin America. Arch Endocrinol Metab 2019;63:462-9. [PubMed]
- Molinaro E, Campopiano MC, Peruzzi L, et al. Active surveillance in papillary thyroid microcarcinoma is feasible and safe: Experience at one Italian single center. J Clin Endocrinol Metab 2020;105:e172-80. [Crossref]
- Koshkina A, Fazelzad R, Sugitani I, et al. Association of patient age with progression of low-risk papillary thyroid carcinoma under active surveillance: a systematic review and meta-analysis. JAMA Otolaryngol Head Neck Surg 2020;146:552-60. [Crossref] [PubMed]
- Miyauchi A, Kudo T, Ito Y, et al. Estimation of the lifetime probability of disease progression of papillary microcarcinoma of the thyroid during active surveillance. Surgery 2018;163:48-52. [Crossref] [PubMed]
- Miyauchi A, Kudo T, Miya A, et al. Prognostic impact of serum thyroglobulin doubling-time under thyrotropin suppression in patients with papillary thyroid carcinoma who underwent total thyroidectomy. Thyroid 2011;21:707-16. [Crossref] [PubMed]
- Miyauchi A, Kudo T, Ito Y, et al. Natural history of papillary thyroid microcarcinoma: Kinetic analyses on tumor volume during active surveillance and before presentation. Surgery 2019;165:25-30. [Crossref] [PubMed]
- Ito Y, Miyauchi A, Kudo T, et al. Kinetic analysis of growth activity in enlarging papillary thyroid microcarcinomas. Thyroid 2019;29:1765-73. [Crossref] [PubMed]
- Ito Y, Miyauchi A, Kudo T, et al. Effects of pregnancy on papillary microcarcinomas of the thyroid re-evaluated in the entire patient series at Kuma Hospital. Thyroid 2016;26:156-60. [Crossref] [PubMed]
- Fukuoka O, Sugitani I, Ebina A, et al. Natural history of asymptomatic papillary thyroid microcarcinoma: Time-dependent changes in calcification and vascularity during active surveillance. World J Surg 2016;40:529-37. [Crossref] [PubMed]
- Oda H, Miyauchi A, Ito Y, et al. Comparison of the costs of active surveillance and immediate surgery in the management of low-risk papillary microcarcinoma of the thyroid. Endocr J 2017;64:59-64. [Crossref] [PubMed]
- Lang BH, Wong CK. A cost-effectiveness comparison between early surgery and non-surgical approach for incidental papillary thyroid microcarcinoma. Eur J Endocrinol 2015;173:367-75. [Crossref] [PubMed]
- Venkatesh S, Pasternak JD, Beninato T, et al. Cost-effectiveness of active surveillance versus hemithyroidectomy for micropapillary thyroid cancer. Surgery 2017;161:116-26. [Crossref] [PubMed]
- Sugitani I, Fujimoto Y, Yamada K. Association between serum thyrotropin concentration and growth of asymptomatic papillary thyroid microcarcinoma. World J Surg 2014;38:673-8. [Crossref] [PubMed]
- Kim HI, Jang HW, Ahn HS, et al. High serum TSH level is associated with progression of papillary thyroid microcarcinoma during active surveillance. J Clin Endocrinol Metab 2018;103:446-51. [Crossref] [PubMed]
- Nickel B, Brito JP, Barratt A, et al. Clinicians' views on management and terminology for papillary thyroid microcarcinoma: a qualitative study. Thyroid 2017;27:661-71. [Crossref] [PubMed]
- Nickel B, Brito JP, Moynihan R, et al. Patients' experiences of diagnosis and management of papillary thyroid microcarcinoma: A qualitative study. BMC Cancer 2018;18:242. [Crossref] [PubMed]
- Ito Y, Miyauchi A, Kudo T, et al. Trends in the implementation of active surveillance for low-risk papillary thyroid microcarcinomas at Kuma Hospital: Gradual increase and heterogeneity in the acceptance of this new management option. Thyroid 2018;28:488-95. [Crossref] [PubMed]
- Jeon MJ, Lee YM, Sung TY, et al. Quality of life in patients with papillary thyroid microcarcinoma managed by active surveillance or lobectomy: a cross-sectional study. Thyroid 2019;29:956-62. [Crossref] [PubMed]
- Kong SH, Ryu J, Kim MJ, et al. Longitudinal assessment of quality of life according to treatment options in low-risk papillary thyroid microcarcinoma patients: active surveillance or immediate surgery (Interim analysis of MAeSTro). Thyroid 2019;29:1089-96. [Crossref] [PubMed]
- Yoshida Y, Horiuchi K, Okamoto T. Patients' view on the management of papillary thyroid microcarcinoma: active surveillance or surgery. Thyroid 2020;30:681-7. [Crossref] [PubMed]
- Davies L, Roman BR, Fukushima M, et al. Patient experience of thyroid cancer active surveillance in Japan. JAMA Otolaryngol Head Neck Surg 2019;145:363-70. [Crossref] [PubMed]
- Brito JP, Moon JH, Zeuren R, et al. Thyroid cancer treatment choice: A pilot study of a tool to facilitate conversations with patients with papillary microcarcinomas considering treatment options. Thyroid 2018;28:1325-31. [Crossref] [PubMed]
- Hirokawa M, Kudo T, Ota H, et al. Pathological characteristics of low-risk papillary thyroid microcarcinoma with progression during active surveillance. Endocr J 2016;63:805-10. [Crossref] [PubMed]
- Yabuta T, Matsuse M, Hirokawa M, et al. TERT promoter mutations were not found in papillary thyroid microcarcinomas that showed disease progression on active surveillance. Thyroid 2017;27:1206-7. [Crossref] [PubMed]
- Haser GC, Tuttle RM, Su HK, et al. Active surveillance for papillary thyroid microcarcinoma: New challenges and opportunities for the health care system. Endocr Pract 2016;22:602-11. [Crossref] [PubMed]
- Miyauchi A, Ito Y. Conservative surveillance management of low-risk papillary thyroid microcarcinoma. Endocrinol Metab Clin North Am 2019;48:215-26. [Crossref] [PubMed]
- Ito Y, Miyauchi A. Active surveillance as first-line management of papillary microcarcinoma. Ann Rev Med 2019;70:369-79. [Crossref] [PubMed]
- Ito Y, Miyauchi A, Oda H. Low-risk papillary microcarcinoma of the thyroid: a review of active surveillance trials. Eur J Surg Oncol 2018;44:307-15. [Crossref] [PubMed]
- Sugitani I, Ito Y, Miyauchi A, et al. Active surveillance versus immediate surgery: questionnaire survey on the current treatment strategy for adult patients with low-risk papillary thyroid microcarcinoma in Japan. Thyroid 2019;29:1563-71. [Crossref] [PubMed]
Cite this article as: Ito Y, Miyauchi A. Active surveillance for low-risk papillary thyroid microcarcinomas. Ann Thyroid 2020;5:17.


