Energy based devices for transoral thyroidectomy
Introduction
Energy based devices (EBDs) are essential accessories in endoscopic and robotic thyroidectomy (1). In a first study by Barczyński et al., 67 patients were randomized into two groups for the minimally invasive video-assisted thyroidectomy (MIVAT) “Miccoli” technique (1): the clip-ligation group (CL-G) and the harmonic scalpel group (HS-G) use. HS-G vs. CL-G procedures were notably shorter (31.4 vs. 47.5 min). Mean blood loss was consequently smaller (12.9 vs. 32.8 mL). Mean scar length positively was shorter (15.6 vs. 21.5 mm), with better cosmetic results. The use of HS was 20–30 euros more expensive. No major complications were observed in both groups (1).
The thyroid surgeon cannot perform a transoral endoscopic thyroidectomy vestibular approach (TOETVA) with the hand ligation of the vessels, both of the mean thyroid vein, or the superior and inferior thyroid vessels (2-9). Intraoperative bleeding control cannot be managed without the aid of the EBD or clip applier (9-14). Furthermore, EBD provide a full range of solutions to support every phase of surgery including tissue and vessel dissection, sealing, cauterization, and ablation applications.
EBD for TOETVA
Accurate haemostasis is imperative when working in a limited space, such as that encountered in TOETVA procedure (2-5). Bleeding may cause conversion to an open procedure (6,7). The following sections will explore the application and limitations of EBD when used in TOETVA.
HARMONIC ACE®+7 Shears with Advanced Hemostasis (Johnson & Johnson, New York, NY, USA)
HARMONIC ACE®+7 Shears is the ultimate refined curved blade design, designed to enable visibility and fine dissection, with fewer instrument exchanges (Figure 1). The refined blade design includes a tapered tip with a proprietary, nonstick coating to enable fast, precise dissection. This EBD seals vessel sizes up to and including 7 mm diameter with hand control button. The adaptive tissue technology of HARMONIC ACE®+7 Shears enables greater surgical precision and performance, provides critical thermal management by dynamically optimizing energy delivery in response to changing tissue conditions. This EBD is available in three shaft lengths: 23, 36, and 45 cm. According to neck length the surgeon will decide for the 23 or 36 cm ones. The EBD provides reduced mist generation helps maintain endoscopic visibility during TOETVA.
ENSEAL® Round Tip Tissue Sealer (Johnson & Johnson, New York, NY, USA)
The ENSEAL® Tissue Sealing Device is indicated for bipolar coagulation and mechanical transection of tissue during both laparoscopic and open procedures (Figure 2).
Thunderbeat (Olympus, Tokyo, Japan)
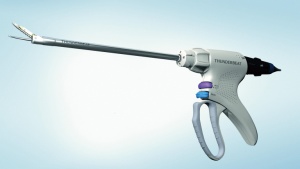
Thunderbeat is a both bipolar and ultrasonic technology device, i.e., surgeons no longer need to choose between rapid dissection and reliable hemostasis when selecting an advanced energy device (Figure 3). The EBD allows the surgeon to simultaneously seal and cut vessels up to and including 7 mm in size with minimal thermal spread, with fewer instrument exchanges. The jaw design provides precise, controlled dissection and fast available bipolar hemostasis without sacrificing grasping ability. The EBD provides reduced mist generation helps maintain endoscopic visibility during TOETVA.
LigaSure™ Maryland jaw (Medtronic, Dublin, Ireland)
LigaSure™ Maryland jaw is a 37 cm laparoscopic sealer and divider (code LF1737). This EBD is a multifunctional device that delivers efficiency and versatility by combining one-step sealing and the functionality of a Maryland dissector, atraumatic grasper, and cold scissors with the reliability of LigaSure™ technology (Figure 4). The design of the LigaSure™ Maryland jaw allows for more efficient transection speed with one-step sealing, allows for minimal steps when sealing and dividing, and enables reduced instrument exchanges. This EBD technology provides a combination of pressure and energy to create vessel fusion. It permanently fuses vessels up to and including 7 mm in diameter and tissue bundles without dissection or isolation. Average seal cycle is 2 to 4 seconds, when used with the ForceTriad™ energy platform. Feedback-controlled response system automatically discontinues energy delivery when the seal cycle is complete, eliminating the guesswork.
EBD safety
Smoke effect
EBD in TOETVA may determine two problems during the procedures: (I) recurrent laryngeal nerve (RLN) thermal injury; (II) smoke effect which determines unsafe, bad vision and loss of time. At present is one of the significant obstacles of EBD use for TOETVA safety, because too much smoke effect disturb the view during important steps. “Smoke effect” is always discussed in the operating room with visiting surgeons. For the smoke effect, it is hard to prove if HARMONIC is better than Thunderbeat or LigaSure™, because it depends certainly on surgeon preferences, his perception of dissection and security and how much use of EBD. Furthermore, the use of one or the other depends on availability in the operating room and the lowest economic offered to the administration of the hospital.
The perception is that smoke effect is generally more at the beginning of TOETVA when creating the workspace, the air pocket. Probably because the working space is smaller, and more muscle needs to dissect. Then the perception is there is less smoke, probably because there is more working space available and the smoke is dissipated, and probably because there is less muscle to coagulate, more anatomical plane.
Possible tips to prevent dense smoke effect are: (I) keep the 5 mm ports valves open; (II) keep the tips of the EBD clean; (III) work on anatomical planes, fascia plane produces less smoke effect than muscle; (IV) keep CO2 at maximum flow; (V) when too much smoke, pull/retract the camera just inside the 10 mm trocar without going out, waiting for the smoke melts.
EBD around the RLN
EBDs are designed to produce minimal temperatures and thermal spread to surrounding tissues. However EBDs are associated with inadvertent thermal transfer to surrounding tissue (15).
Recently, authors have alert that the temperature from EBD may cause laryngeal nerves injury, resulting in vocal cord palsy (15). Standardized experimental studies proved that when EBDs are activated near the RLNs, the heat produced can be conducted through the tissues to the nerve and cause thermal trauma and risk of permanent function deficit (15).
De facto, thermal injury is the second most common mechanism of RLN damage after traction injury during thyroidectomy (15).
Furthermore, the effectiveness of saline irrigation to reduce the chance of nerve root injury during EBD application has not been investigated, despite irrigation having been shown to decrease the temperature.
Conclusions
Currently there are no specific studies that evaluate or compare EBD in TOETVA (8-10). Current EBD developed meet stringent design specification and performance requirements for most of laparoscopic or thoracoscopic procedures. Unfortunately there are no EBDs with precise design specifications and requirements specifically developed for the TOETVA procedure (9).
The ideal EBD may present low temperatures proprieties in order not to damage the overlying skin of the airpoket, or other vital structures such as RLN and parathyroid glands. The ideal EBD should produce little or no smoke effect during their application, to maintain perfect endoscopic view and not to longer the operative time.
Considering the wide adaption of TOETVA, a full range of solutions to support every phase of the thyroid dissection for access instruments is required (11,12). Endoscopic thyroidectomy and TOETVA in particular is an exciting opportunity for improved techniques and accessories to improve EBD outcomes (13,14).
Future perspective for EBD in TOETVA is a neuromodulation product category that can offer a comprehensive breadth of technologies and capabilities, ensuring the surgeon that receives an EBD instruments superior quality in an efficient, cost-effective, repeatable/reusable, dissecting, coagulating, cutting and with neural monitoring capabilities.
Acknowledgments
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editors (Anuwong Angoon, Hoon Yub Kim, Ralph P. Tufano and Gianlorenzo Dionigi) for the series “Transoral Thyroidectomy” published in Annals of Thyroid. The article has undergone external peer review.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/aot.2018.01.02). The series “Transoral Thyroidectomy” was commissioned by the editorial office without any funding or sponsorship. Gianlorenzo Dionigi served as the unpaid Guest Editor of the series and serves as an unpaid editorial board member of Annals of Thyroid from Mar. 2017 to Feb. 2019. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the manuscript and ensure that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The protocol, site-specific informed consent forms, participant education and recruitment materials, and other requested documents and any subsequent modifications were reviewed and approved by Ethical Review Body of the University of Messina. Informed consent was obtained from all individual participants included in the study.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Barczyński M, Konturek A, Cichoń S. Minimally invasive video-assisted thyreoidectomy (MIVAT) with and without use of harmonic scalpel--a randomized study. Langenbecks Arch Surg 2008;393:647-54. [Crossref] [PubMed]
- Chai YJ, Kim HY, Kim HK, et al. Comparative analysis of 2 robotic thyroidectomy procedures: Transoral versus bilateral axillo-breast approach. Head Neck 2017; [Epub ahead of print]. [Crossref] [PubMed]
- Dionigi G, Tufano RP, Russell J, et al. Transoral thyroidectomy: advantages and limitations. J Endocrinol Invest 2017;40:1259-63. [Crossref] [PubMed]
- Dionigi G, Chai YJ, Tufano RP, et al. Transoral endoscopic thyroidectomy via a vestibular approach: why and how? Endocrine 2018;59:275-9. [PubMed]
- Chai YJ, Chung JK, Anuwong A, et al. Transoral endoscopic thyroidectomy for papillary thyroid microcarcinoma: initial experience of a single surgeon. Ann Surg Treat Res 2017;93:70-5. [Crossref] [PubMed]
- Russell JO, Clark J, Noureldine SI, et al. Transoral thyroidectomy and parathyroidectomy - A North American series of robotic and endoscopic transoral approaches to the central neck. Oral Oncol 2017;71:75-80. [Crossref] [PubMed]
- Kim HY, Chai YJ, Dionigi G, et al. Transoral robotic thyroidectomy: lessons learned from an initial consecutive series of 24 patients. Surg Endosc 2018;32:688-94. [Crossref] [PubMed]
- Anuwong A, Sasanakietkul T, Jitpratoom P, et al. Transoral endoscopic thyroidectomy vestibular approach (TOETVA): indications, techniques and results. Surg Endosc 2018;32:456-65. [Crossref] [PubMed]
- Anuwong A, Kim HY, Dionigi G. Transoral endoscopic thyroidectomy using vestibular approach: updates and evidences. Gland Surg 2017;6:277-84. [Crossref] [PubMed]
- Dionigi G, Lavazza M, Wu CW, et al. Transoral thyroidectomy: why is it needed? Gland Surg 2017;6:272-6. [Crossref] [PubMed]
- Dionigi G, Bacuzzi A, Lavazza M, et al. Transoral endoscopic thyroidectomy: preliminary experience in Italy. Updates Surg 2017;69:225-34. [Crossref] [PubMed]
- Dionigi G, Lavazza M, Bacuzzi A, et al. Transoral Endoscopic Thyroidectomy Vestibular Approach (TOETVA): From A to Z. Surg Technol Int 2017;30:103-12. [PubMed]
- Dionigi G, Bacuzzi A, Lavazza M, et al. Transoral endoscopic thyroidectomy via vestibular approach: operative steps and video. Gland Surg 2016;5:625-7. [Crossref] [PubMed]
- Dionigi G, Rovera F, Boni L. Commentary on transoral access for endoscopic thyroid resection: Witzel K, von Rahden BH, Kaminski C, Stein HJ (2008) Transoral access for endoscopic thyroid resection. Surg Endosc 22(8):1871-1875. Surg Endosc 2009;23:454-5; discussion 456. [Crossref] [PubMed]
- Dionigi G. Energy based devices and recurrent laryngeal nerve injury: the need for safer instruments. Langenbecks Arch Surg 2009;394:579-80; author reply 581-6. [Crossref] [PubMed]
Cite this article as: Wu CW, Rizzo AG, Bartolo V, Pergolizzi FP, Marullo M, Cancellieri A, Melita G, Catalfamo A, Dionigi G. Energy based devices for transoral thyroidectomy. Ann Thyroid 2018;3:4.